Children and rare neurological diseases
“It’s an exciting time in pediatric neurology. Scientific knowledge is rapidly expanding, our ability to make specific diagnoses is improving, and life-changing therapies are emerging. Each day, there is an imperative to advance this progress in the field.”
—Dr. Erika Augustine
 Children and rare neurological diseases
Children and rare neurological diseases
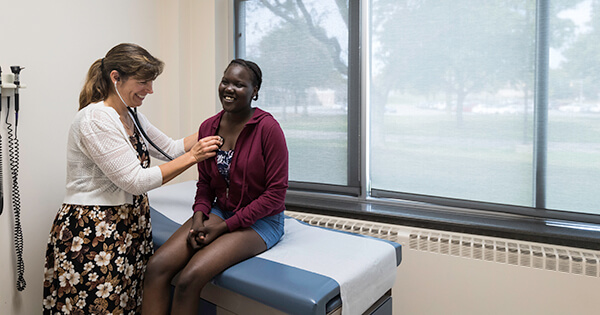
Erika Augustine ’03M (MD), ’10M (FLW), ’14 (MS-TR) is a pediatric neurologist who works with children with rare neurological diseases. As both a researcher and a clinician, she is focused on bringing forward new treatments to help children function better, improve their quality of life, and, ultimately, survive longer.
Most children with rare neurological diseases suffer from many symptoms at the same time, like problems with moving too much or too little, muscle weakness, seizures, problems with vision or hearing, and other problems with the senses.
“It’s incredibly frustrating when we aren’t able to improve the symptoms that happen.” says Augustine. “In so many ways, medicine is progressing but in other ways we haven’t really even scratched the surface.”
That’s starting to change though. Parkinson’s disease, Alzheimer’s disease, Huntington disease, stroke, and other neurological conditions are gaining more and more national attention. This is the era of the brain, Augustine says, and unlocking its mysteries means improving, lengthening, and even saving millions of lives, both young and old.
Rochester is well poised for this work.
“We have some of the most highly regarded neurologists here,” adds Augustine. This type of expertise drew Augustine to Rochester for both medical school and, later, for a dual fellowship in pediatric movement disorders and experimental therapeutics.
“In my work, there are days where we see patients struggle to do essential activities like sitting, communicating, or being able to play or work,” she says. “Although I can sometimes help manage symptoms, there is often little any of us can do to extend lives. This is changing, and this is where I want to focus.”
Since she joined the University of Rochester Medical Center (URMC) in 2008, Augustine has worked with those in pediatric and adult neurology, in the Center for Health and Technology and others in the Clinical and Translational Science Institute. In the last few years, she and her colleagues have seen increased collaboration with industry and academic centers, too, to bring forth new therapies and trials.
Augustine and her colleagues are also using video conferencing more often for care and research with more frequency. Asked why, she says that it makes research fair and equitable—everyone can participate. It provides ways to get information in a timely manner across various geographies and demographics. Getting that diverse information is important, too. “With rare diseases, everyone’s information matters,” she adds. “We need to constantly innovate and use technology in new ways to expand our knowledge.”
Such collaboration and innovation are keys to advancing discovery, too. And hope.
Dr. Erika Augustine is one of URMC’s 3,000 researchers. In the video above, she talks about juvenile Batten disease and why she became a physician.
Help us help more children
You can help by supporting neuromedicine, research, and care at the University of Rochester Medical Center. Please contact James O’Brien, Senior Director of Advancement for URMC’s Ernest J. Del Monte Institute for Neuroscience, at (585) 276-6877.
—Kristine Thompson, January 2018